Difficult coworker
They told you about the caseloads. The paperwork. The compassion fatigue and the clients who don’t want to be there. They prepared you—sort of—for the hard stuff that comes with the work itself.
But nobody sat you down and said: sometimes the hardest part of this job is the person sitting ten feet away from you.

The one who doesn’t pull their weight. The one who gossips. The one who’s been there for fifteen years and treats every new hire like a personal threat. The one who talks about boundaries in session but doesn’t have a single one at the office.
And here’s the part that makes it really complicated: sometimes it’s someone you genuinely care about.
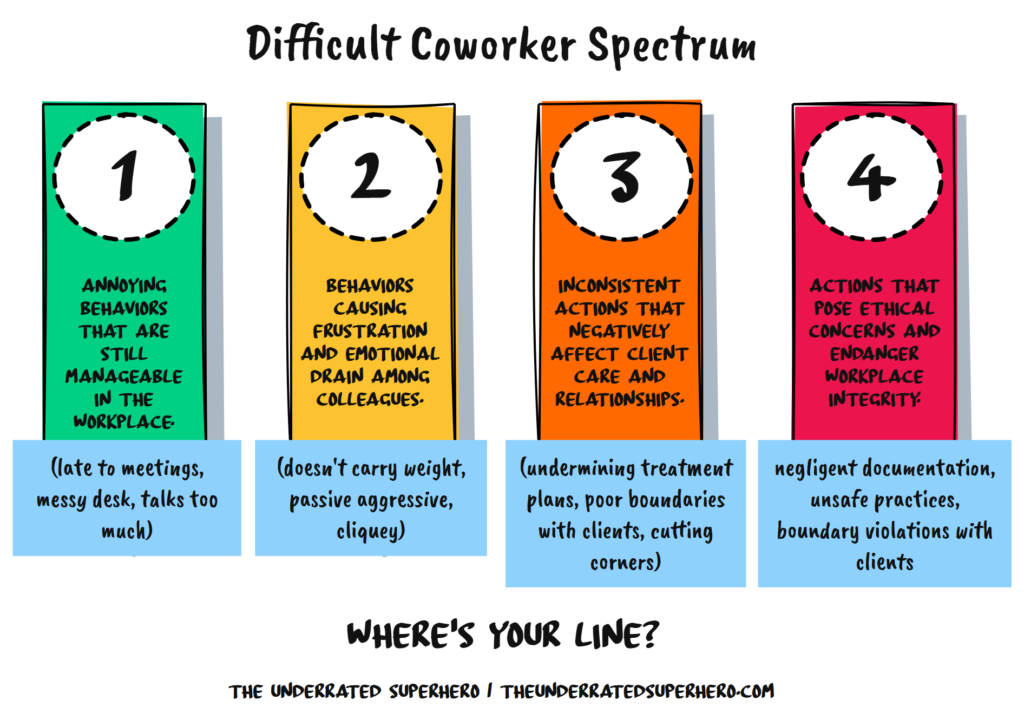
or ignoring a 4 because theyre likable
📚 This is Blog #20 in the New Clinician Survival Kit Series (Click to explore the series)
Weekly honest support for the struggles every clinician faces: “I hate group therapy.” “I can’t do this.” “My client hates me.” “I’m making it worse.” “I can’t say no.” “They’re going to report me.” “I’m too tired to care.” “What do I even say?” “I don’t know enough.” “They keep relapsing.” “Am I documenting wrong?” “My supervisor doesn’t get it.” “I can’t handle this caseload.” “Nobody told me about the paperwork.” “I don’t like my client.” “My client’s cute.” “My client likes me.” “I got a complaint.” “I want to quit.” “My coworker is terrible.”
These aren’t signs you’re failing. They’re signs you’re human.
You Know These Difficult Coworkers

If you’ve been in clinical work for more than five minutes, you’ve met at least one. Probably three.
The one who doesn’t carry their weight
Their notes are always late. They leave early. They somehow have half your caseload but twice your complaints. Meanwhile you’re staying late, picking up groups they were supposed to run, auditing charts they were supposed to maintain, building tools to help the team get better. And nobody—nobody—seems to notice the gap.
You end up carrying the team. Not because anyone asked. Because if you don’t, it doesn’t get done. You move through your waitlist faster, manage groups more efficiently, get through assessments quicker. And at some point you look up and realize you’re not just doing your job. You’re doing theirs too.
The gossip
This one’s tricky because sometimes they’re fun. They know everything about everyone. They tell you things about other staff like they’re trusting you with something sacred. And for a while it feels like connection. Like you’re on the inside.
Until you’re on the other side of it.
I’ve seen bosses—actual bosses—talk about other clinicians behind their backs. One day they’re confiding in you about someone’s performance, and the next day you’re lying awake wondering what they’re saying about you down the hall. Because if they’ll do it with you, they’ll do it about you. That’s not pessimism. That’s just math.
The clinically questionable one
This one keeps you up at night. You see them doing the bare minimum. Not challenging clients in productive ways. Letting boundaries get so porous there’s barely a therapeutic frame left. You watch it happen and you want to say something, but you’re not their supervisor and it’s technically not your lane.
Except those are real people sitting in that office getting subpar care. And you know it.
The gatekeeper
They’ve been there forever. They’ve got relationships with clients, staff, leadership. And they look at you—new, doing things differently—and they don’t like it.
I worked in residential once where staff had formed tight bonds with each other and with the kids. I came in trying to hold structure and expectations, and that made me the outsider. Because the path of least resistance was to let things slide, and I wouldn’t do that. You can’t just do the least to be liked by colleagues. But when those colleagues are the ones who decide whether you feel supported at work? That’s a lonely realization.

When It’s Someone You Like

This is the one that messes with your head.
Sometimes the difficult coworker isn’t someone you can’t stand. It’s your friend. The person you eat lunch with. The one you vent to after hard sessions. Maybe you hang out outside work.
And they’re also the one who isn’t pulling their weight.
You don’t want to resent them. But you do. A little. Because you’re staying late while they’re heading out. You’re picking up the stuff nobody acknowledges as slack. And you can’t bring it up without risking a friendship that’s one of the only things making this job survivable.
So you swallow it.
And I don’t have a clean answer for this one. I really don’t. If you say something, the dynamic shifts. If you don’t, the resentment grows. And in clinical work, having people who have your back isn’t a luxury—it’s survival. Research on burnout in mental health settings consistently points to coworker support as one of the strongest protective factors against emotional exhaustion. Losing that over a conversation about chart audits feels like a bad trade.
But here’s what I’ve learned, and I’m still learning it honestly: resentment is quieter than conflict but it’s more corrosive. If you’re carrying someone professionally while pretending you’re not, the friendship is already strained. You just haven’t named it yet.

Your Clients Can See It
This is the part people forget. Or don’t want to think about.
Coworker tension doesn’t stay in the staff room. Clients notice when clinicians aren’t on the same page. They feel it. Especially—and I mean especially—clients who grew up in chaotic or dysfunctional systems. Those folks have been reading rooms since they were kids. They know when something’s off before you do.
And when clinicians aren’t communicating? Clients figure it out fast. They get one answer from you and a different one from your coworker. They play the gaps—not because they’re inherently manipulative, but because inconsistency is an opening and some of our clients are really, really good at finding openings.
Clients get annoyed repeating themselves. Getting different directions from different staff. Hearing one thing in group on Tuesday and something contradictory in individual on Thursday. That’s not their problem. That’s a team that isn’t talking to each other.

A 2025 study from Workplace Options found that interpersonal conflict is now one of the top three workplace concerns across industries, and healthcare settings are being hit particularly hard. That tracks. When your coworker is draining you before your first client even walks in, the care suffers. Period.
The Judgment Problem
Can I be honest about something?
Therapists, as a group, are judgmental. I know we’re supposed to be the empathetic ones. The nonjudgmental listeners. And we are—with our clients. With each other? Not always.
My sister is a director of academic advising at a public university. She works with BIPOC students — a lot of whom are drawn to helping professions. She used to recommend counseling. She doesn’t anymore. Not because of the clients. Because of what she’s heard from me, and from her own students, about how colleagues and supervisors treat each other in this field. When someone whose whole job is guiding students into careers stops sending them into yours, that should tell us something.
Spend five minutes in any online group for therapists. Watch what happens when someone asks a genuine question about something they’re unsure about. Watch the pile-on. Watch someone share a real struggle and get judged for it instead of supported. It’s gotten to the point where people now preface posts with “please be kind” and “please be nice” before asking for help.

We Got into This Field Because of Our Own Stuff
I think a lot of this comes from the fact that many of us got into this field because of our own stuff. And I’m not saying that critically—the wound is often what makes us effective. But when we haven’t done our own work? When we’re still dragging around unprocessed trauma and poor boundaries? That stuff leaks out sideways. Onto colleagues. Into the break room. Into staffing meetings where everyone’s trying to be the smartest person in the room instead of the most helpful. Research from the Society for the Advancement of Psychotherapy has started naming this directly—that the mental health field sometimes perpetuates the very dysfunction it treats.
This Is Not Just My Experience
In fifteen years I have heard so many stories. Bosses who weaponize information. Colleagues who sabotage over personal grudges. Supervisors who preach ethics in the morning and gossip at lunch. And I don’t think these are outliers. When you hear the same patterns from clinicians across different settings, different states, different populations—that’s not anecdotal anymore. That’s systemic.
And the numbers back it up. A recent survey found 48% of behavioral health workers have considered leaving their jobs due to stress and workload. Staff turnover in substance abuse treatment settings runs as high as 50% in some contexts, with an average of about 32% annually for counselors. You want to know why? It’s not just the clients. It’s not just the pay. A lot of people leave because the workplace itself is intolerable.
Venting vs. Toxicity
Venting is fine. Healthy, even. You need to be able to say “I’m so frustrated with this person” to someone you trust. That’s normal. That’s how you don’t explode.
But there’s a line.
It crosses into unhealthy when it gets personal. When it starts causing friction that bleeds into the team. When rumors start. When people pick sides. When the venting turns into a campaign.
Healthy sounds like: “I’m frustrated that I keep ending up with extra work. I need to figure out how to address this.”
Toxic sounds like: “Let me tell you what she did now—and did you hear what she said to the client in Room 3?”
One is processing. The other is performing. And if you’re being honest with yourself, you know the difference. You’ve probably been on both sides of it. I know I have.
Venting: Healthy vs. Toxic
One helps you process. The other poisons the room.
Know the difference. Protect your energy. Protect your team.
The Underrated Superhero · theunderratedsuperhero.comWhen a Difficult Coworker Crosses Into Dangerous
A coworker can be lazy. Boring. Standoffish. Frustrating. All of that is survivable. You don’t have to like everyone you work with.
But when it crosses into negligent, unsafe, or aggressive—that’s a different conversation.
Negligent means clients are at risk. Documentation isn’t happening. Safety protocols are being skipped. People are falling through cracks that have no business existing. That’s not a personality clash. That’s an ethical issue.
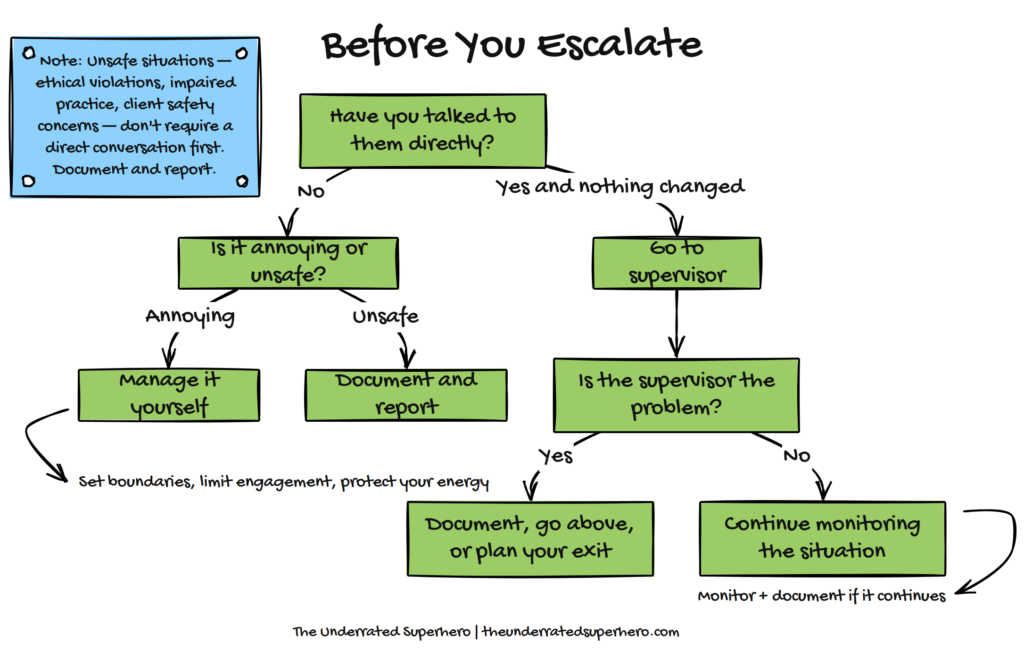
And if you see it, you have an obligation to say something. Not to the break room. To a supervisor. To compliance. To whatever reporting structure exists in your setting. That’s not being a snitch. That’s being a clinician.
And if the supervisor IS the problem? Document. Go above them. Or start planning your exit. I’ve written about knowing when it’s time to leave—sometimes the healthiest move is walking away from a culture that refuses to change.
So What Do You Do About a Difficult Coworker
Find Your Line
A quick gut check. No scoring, no diagnosis — just honesty with yourself.
“Find your line. When someone crosses it, respond like a clinician — with boundaries, not gossip.”
If you came to me and said “I can’t stand my coworker,” here’s what I’d probably say. And I’d probably say it while we were both complaining about parking.
It’s normal. Like, completely normal. Clinical settings are a pressure cooker. You’re already emotionally spent from the work, and then you’ve got to navigate personalities with people who are also emotionally spent.
Figure out what you can control. You can’t make someone a better clinician. You can’t stop someone from gossiping. You can protect your own practice, maintain your own standards, and choose what you participate in. That’s not nothing.
Don't compromise your integrity to fit in. I've been the person who held boundaries when everyone else relaxed them. It made me unpopular. And I won't pretend I handled every situation perfectly — I didn't. But the boundaries I held? I don't regret those. The ones I let slide to keep the peace? Those are the ones that kept me up at night.
Know when to escalate. Personality conflicts don’t need HR. Clinical negligence does. Complaints are scary, but sometimes they’re necessary. Learn the difference between annoying and reportable. Act accordingly.
Know when to leave. If the environment is genuinely toxic—gossip is rampant, leadership enables it, you’re spending more energy managing the workplace than your caseload—that’s not a coworker problem. That’s a culture problem. And sometimes the healthiest thing is to go.
Part of the Job
The difficult coworker is part of the job. I wish it weren’t. I wish every treatment setting was staffed with self-aware, boundaries, professionally mature humans who’ve done their own therapy and come to work ready to collaborate.
That’s not what happens.
What happens is a mix. Good people having terrible days. Burned-out people phoning it in. Wounded people projecting their stuff sideways. And occasionally, genuinely harmful people in positions they shouldn’t occupy. We're already short-staffed enough as it is - projections say over 100,000 addiction counselors short by 2037. We can’t afford to lose good clinicians because of bad workplace dynamics.
You can’t fix your coworker. That’s not your job. Your job is to protect your clients, maintain your standards, and figure out where your line is—the line between “this is annoying, but I can manage” and “this is affecting my work, and something has to change.”
Find your line. When someone crosses it, respond like a clinician: with documentation, not drama. With boundaries, not gossip.
You went into this field to help people. Don’t let the person in the next office make you forget that.

Next in the series: "Nobody Respects What We Do" — because the profession that's supposed to heal people can barely take care of the people doing the healing.
This is Blog #20 in the New Clinician Survival Kit Series by The Underrated Superhero. If this hit close to home, you're not alone. Follow along for more real talk about surviving your first years in clinical work.
Until Next Week | The Underrated Superhero
© 2026 The Underrated Superhero LLC. All Rights Reserved.
📖 External Resources & Research
- 🔗 Burnout in Mental Health Services: A Review of the Problem and Its Remediation — PMC — Research showing coworker support is one of the strongest protective factors against emotional exhaustion and turnover in clinical settings
- 🔗 Abuse and Burnout in Health Profession Workplace Environments — Society for the Advancement of Psychotherapy — Research naming how the mental health field sometimes perpetuates the very dysfunction it treats, including toxic training environments and workplace harassment
- 🔗 Workplace Stress, Conflict and Performance Pressure Are Rising in 2025 — Managed Healthcare Executive — 2025 study finding interpersonal conflict is now a top three workplace concern, with healthcare settings hit especially hard
- 🔗 SAMHSA: Quality Assurance in Substance Abuse Treatment Facilities — Research showing counselor turnover as high as 50% in some settings, with annual averages around 32%
- 🔗 HRSA: State of the Behavioral Health Workforce, 2025 — Federal brief projecting shortages of over 100,000 addiction counselors by 2037, with burnout and workplace dynamics driving attrition
- 🔗 2025 Federal Addiction & Mental Health Policy — BehaveHealth — Survey finding 48% of behavioral health workers have considered leaving their jobs due to stress and workload
📌 From This Series
- 🔗 Blog #5: "I Can't Say No" — Boundary-setting and the cost of people-pleasing
- 🔗 Blog #7: "I'm Too Tired to Care" — When exhaustion stops being a bad week and starts being your baseline
- 🔗 Blog #12: "My Supervisor Doesn't Get It" — When the person who's supposed to help can't
- 🔗 Blog #13: "I Can't Handle This Caseload" — Drowning in clients and running out of air
- 🔗 Blog #18: "I Got a Complaint" — Handling grievances without spiraling
- 🔗 Blog #19: "I Want to Quit" — When burnout becomes a career question

