Part of the Justice-Involved Treatment Mastery Series
Your client just had a positive drug test.
You’re looking at the results. They’re looking at you. And both of you are thinking the same thing: there’s a court date coming.
Here’s what most clinicians do in this moment. They panic. They go straight to the consequences. We need to call your PO. What’s the judge going to say. You know what this means for your case.
And just like that, the clinical moment is gone. You’ve turned a therapeutic event into an administrative one. You’ve become part of the system your client already doesn’t trust.
I get it. The pressure is real. NIDA tells us relapse rates for substance use disorders sit between 40 and 60 percent — comparable to relapse rates for hypertension and asthma (NIDA, 2020). For justice-involved clients specifically, the research paints an even starker picture: 68% of drug offenders are rearrested within three years of release from prison (Belenko, 2013). Relapse isn’t a surprise. It’s a statistical likelihood. And if we’re not prepared for it, we’re not doing our jobs.
So. What does managing relapse actually look like when the court is watching?
Managing Relapse Starts Before You Pick Up the Phone
When a client relapses — whether they tell you or the drug test does — the first words out of your mouth set the tone for everything that follows. Everything.
If you lead with court consequences, here’s what you’ve just communicated: the legal system matters more than the person sitting in front of you. And this client — who probably already feels like the entire world sees them as a case number — just got that confirmed by the one person who was supposed to be different.
So don’t do that.
Start with what the relapse means for their goals. Not the court’s goals. Not probation’s goals. Theirs.
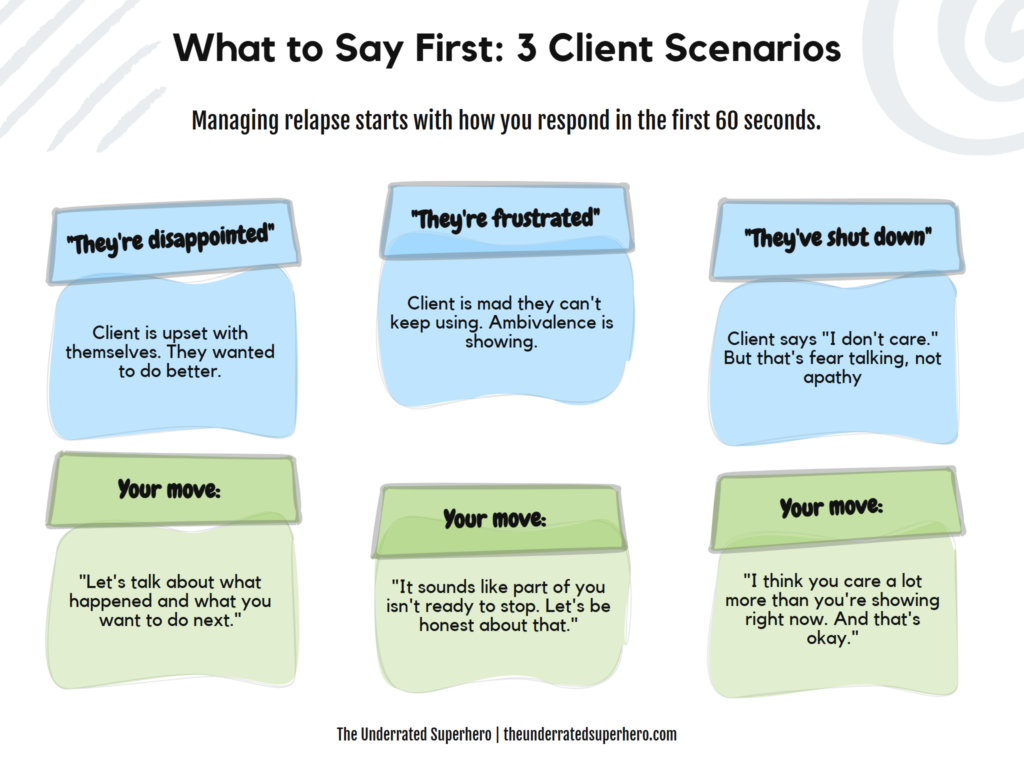
And here’s the thing people forget: court-required abstinence isn’t always the client’s individual goal. That matters. A lot. Because a client who’s disappointed in themselves after a relapse is in a completely different place than a client who’s frustrated they can’t keep using. And both of those are different from the client who’s so terrified of going to jail that they’ve shut down into an “I don’t care” posture — because caring feels too dangerous right now.
Each of those tells you something critical. Disappointed? That’s internal motivation. Work with it. Frustrated? That’s ambivalence. Meet it where it is. Shut down? That’s fear dressed up as apathy. Name it.
You won’t get to any of that information if your opening line is about probation.
Look: You can’t address the relapse without eventually addressing the court stuff. I’m not saying ignore it. I’m saying the order matters. Clinical first. Administrative second. What this means for their recovery comes before what this means for their case. Every time.
Not Every Slip Requires a Phone Call
This section is going to make some people uncomfortable. Good. It needs to be said.
There’s a difference between a slip and a full-blown relapse. Clinically, these are not the same thing. But the court? The court treats them the same. Any substance use is a violation. Period. No room for nuance.
Which is exactly why clinicians need to be careful about just reporting everything.
The ACA Code of Ethics is built on five core principles, and one of them is nonmaleficence — first, do no harm (ACA, 2014). That principle doesn’t evaporate because your client is on probation. A single slip doesn’t always have to be reported to the court. I use my clinical judgment. And yes, technically all substance use should be disclosed. But sometimes reporting every minor slip to probation does not benefit the client’s treatment outcome. Sometimes it actively destroys it.
Think about it. A client who knows that one beer on a bad night means immediate incarceration isn’t going to tell you about the bad night. They’re going to stop being honest with you. And a client who stops being honest with their counselor? That’s a client in real danger. SAMHSA’s TIP 44 on substance abuse treatment in criminal justice settings emphasizes that the therapeutic alliance is one of the strongest predictors of treatment outcomes — and nothing kills an alliance faster than a client who feels their counselor is a surveillance extension of the court (SAMHSA, 2005).
When Clinical Judgment Gets Complicated
Now. If the client isn’t able or willing to try again toward their goals, that changes things. I can’t ignore a sustained lack of progress. But they need to be given time. Recovery is not linear. The legal system’s expectation of linear progress doesn’t make it so, no matter how many times they put it in a court order.
The key question isn’t did they use. The key question is what does this use tell me about where they are, and what do they need next?
Remember: The court treats every slip like a full relapse. That doesn’t mean you have to. Your clinical judgment exists for a reason — use it.
When You Do Report: Have the Plan Before the Phone Call
When it’s a full relapse — a return to continuous use, not a one-time slip — the conversation with the court is happening whether you want it to or not.
So here’s how I handle it.
First. If the client was honest with you about what happened, thank them. Out loud. I know that sounds basic but a lot of clinicians skip it. That client just told you something that could send them to jail. The courage that takes — especially for someone who’s been burned by every system they’ve ever touched — deserves to be acknowledged. Honesty in that context is a clinical win even if the content isn’t what anyone wanted to hear.
If it was a positive drug test rather than self-report, that’s a different conversation. But it’s still a conversation, not an interrogation.
Build the Plan, Then Make the Call
Second. Develop the plan before anyone picks up the phone. What does the client need? More sessions? A higher level of care? Different interventions? Additional supports? Get specific. Write it down. This isn’t the time for vague treatment plan language.
Third — and this is the part that changes everything — have the client make the call themselves.
I would have my clients call their probation officer and be honest about what happened. Better the PO hears it from the client than from me in a report. But here’s what makes this work: by the time they pick up that phone, they already have a plan. They’re not just reporting a failure. They’re reporting a failure and telling the PO what they’re doing about it.
“I relapsed” puts the client in a passive, powerless position. “I relapsed, and my counselor and I are increasing sessions to twice a week and adding a relapse prevention group” — that’s a completely different conversation. Research on drug courts backs this up: graduated therapeutic responses to substance use are more effective at reducing recidivism than purely punitive sanctions (Marlowe, 2012; Gottfredson et al., 2007). Probation officers and judges respond to accountability paired with action. Not always. But more often than most clinicians expect.
The shift: “I relapsed” is a confession. “I relapsed and here’s what I’m doing about it” is accountability. Help your client get to the second version before they ever pick up the phone.
The Plan Before the Relapse

I want to tell you something I wish someone had told me earlier in my career.
Years ago, when I was working in IOP, I wanted to bring a relapse plan into group. Not a relapse prevention plan — a relapse response plan. Something that answers: if you relapse, what happens next? Who do you call? What do you tell your PO? What increased supports do you agree to?
A colleague told me I’d be giving them permission to relapse.
I wasn’t confident enough to push back at that point. So I dropped it. And I regret that.
Because here’s what I know now. Not having a plan doesn’t prevent relapse. It just guarantees that when it happens — and for many justice-involved clients it will happen, the research is clear on this — everyone panics. The client panics because they don’t know what to do. The counselor panics because there’s no protocol. And in that panic, bad decisions get made. Clients disappear. Counselors over-report out of fear. The court steps in with a hammer when what was needed was a recalibration.
The National Drug Court Institute has noted that relapse should be treated as an opportunity to reevaluate and modify a participant’s treatment plan based on factors that may have contributed to it — not as an automatic program failure (NDCI, 2011). That’s not a soft take. That’s evidence-based practice.
What a Pre-Relapse Safety Plan Actually Looks Like
A pre-relapse safety plan is not permission to use. It’s harm reduction at its most practical. It says: we know recovery isn’t linear, and we’re going to be prepared for that reality rather than pretending it doesn’t exist.
Build it early. Build it when the client is stable, thinking clearly, and the stakes feel manageable. Not in the middle of a crisis when everyone’s operating from fear.
Say it louder: Not having a plan doesn’t prevent relapse. It just guarantees that when it happens, nobody knows what to do.
When the System Pushes Back on You
At some point — and I need you to hear this — you will make the right clinical call and have somebody in the legal system question your judgment.
It might be a PO. It might be an attorney. Might be a judge.
I’ve been there. I was pressing for increased interventions when the system wanted to terminate a client, and the attorney started making comments. Things like “maybe we need to talk to another provider.” That’s not a clinical conversation. That’s a power move designed to make you doubt yourself and fall in line.
Don’t.
You are the treatment professional. The attorney is not. The PO is not. The judge is not. They have expertise in their domains. You have expertise in yours. SAMHSA’s TIP 44 lays this out explicitly: effective treatment in criminal justice settings requires genuine collaboration between systems — not one system overriding the other (SAMHSA, 2005). Collaboration is essential. But capitulation is not collaboration.
Three Things That Protect You When It Gets Heated
When pushback comes, here’s what protects you:
Frame everything in shared outcomes. The court wants reduced recidivism and public safety. Those are your goals too. When you advocate for keeping a client in treatment post-relapse, you’re not being soft. You’re pursuing the same outcome the court wants through a method that actually works. Research from NIJ’s Multisite Adult Drug Court Evaluation confirmed that programs focused on treatment retention over punitive responses produce significantly better outcomes in both drug use and criminal behavior (NIJ, 2011). Say it that way.
Know your ethics code. When an attorney implies you should change your clinical opinion to match their preference, that’s not how any of this works. The ACA Code of Ethics is clear: counselors avoid actions that cause harm, and that includes capitulating to external pressure that compromises clinical judgment (ACA, 2014). You don’t need to quote the code in court. You just need to know it’s behind you.

Bottom line: Collaboration means working together toward shared goals. It doesn’t mean changing your clinical opinion because a lawyer got loud.
Managing Relapse in Your Documentation: Same Event, Completely Different Story
If you read Article 4 in this series (“Documentation That Satisfies Courts AND Supports Recovery”), you already know this: how you write about a client matters as much as what you write. Nowhere is that more true than when you’re documenting a relapse.
The difference between documentation that triggers a violation and documentation that shows ongoing clinical work? It’s framing. Same facts. Different narrative.
This is what gets your client locked up:
“Client reported using methamphetamine over the weekend. This is a violation of his probation terms. PO notified.”
This is what keeps them in treatment:
“Client self-reported substance use over the weekend, demonstrating continued engagement in the therapeutic process and willingness to address setbacks honestly. Clinical assessment indicates this represents a lapse in the context of ongoing recovery efforts rather than a return to baseline use patterns. Treatment plan adjusted to include increased session frequency (2x/week) and addition of relapse prevention skills group. Client expressed disappointment in the lapse and identified specific triggers to address in upcoming sessions. Client and clinician collaboratively developed an updated safety plan. PO contacted with clinical summary and updated treatment recommendations.”
Same event. Same facts. The first version tells the court your client failed. The second tells the court your client is actively engaged in treatment that includes honest self-reporting, clinical assessment, and responsive intervention. Both are true. Only one protects your client while keeping your integrity intact.
And this isn’t spin. This is accurate clinical documentation. The second version reflects what actually happened in session. The first version just reports an event. If all you’re doing is reporting events, you’re not documenting treatment. You’re keeping a log.
Check yourself: If your progress notes only report events, you’re not documenting treatment. You’re keeping a log.
So What Kind of Counselor Are You Going to Be?
The counselor who panics, over-reports everything, and lets the legal system run the clinical response? That counselor’s clients end up back in a cell. The research is consistent on this: punitive-only responses to substance use in justice settings increase recidivism rather than reducing it (Belenko, 2013; NIJ, 2011).
The counselor who approaches managing relapse as clinical work — not damage control — is the counselor whose clients actually have a shot.
You can honor the court’s expectations and your client’s humanity at the same time. Nobody said it was easy. But you didn’t get into this work because it was easy.
📁 This Month’s Toolkit: Log in or create a free account to download from the Justice-Involved Mastery Page
Article 6 comes with four downloadable tools for managing relapse in justice-involved settings — the biggest resource drop in the series so far:
1. Relapse Response Decision Tree — Visual flowchart for the moment it happens. Branches for self-reported vs. positive test, slip vs. full relapse, client engagement level, and clinical actions at each point.
2. Slip vs. Relapse Assessment Quick Reference — One-page guide. How to differentiate them, what questions to ask, how each impacts court reporting decisions, and the ethical framework for using clinical judgment.
3. “What to Say When” Script Card — Pocket-sized. Actual language for the hardest moments: client admits relapse, when you’re sitting with a positive drug test, client calls their PO, attorney pushes back on your clinical judgment.
4. Pre-Relapse Safety Planning Worksheet — Build this with your client before anything goes wrong. Who they call, what they tell their PO, what increased interventions they agree to, step-by-step plan for getting back on track.
This is Article 6 of the Justice-Involved Treatment Mastery Series — an 8-month deep dive for clinicians working with mandated clients, drug court participants, and anyone navigating treatment in justice settings.
Missed the earlier articles? Start with Article 1: Beyond Court Compliance →
Previous articles in this series:
- Month 1: Beyond Court Compliance: Harm Reduction with Mandated Clients →
- Month 2: When the Judge Says Abstinence but Evidence Says Harm Reduction →
- Month 3: From Compliance to Care: Why Justice-Involved Clients Need a Different Approach →
- Month 4: Documentation That Satisfies Courts AND Supports Recovery →
- Month 5: Motivational Interviewing for Mandated Clients
Browse the full Justice-Involved Treatment Mastery hub →
Not a member yet? Create a free account to access resources →
References
- American Counseling Association. (2014). 2014 ACA Code of Ethics. Alexandria, VA: Author. https://www.counseling.org/resources/ethics
- Belenko, S. (2013). Treating substance use disorders in the criminal justice system. Current Psychiatry Reports, 15(11), 414. https://pmc.ncbi.nlm.nih.gov/articles/PMC3859122/
- Coviello, D. M., Zanis, D. A., Wesnoski, S. A., & Alterman, A. I. (2013). Does mandating offenders to treatment improve completion rates? Journal of Substance Abuse Treatment, 44(4), 417-425. https://pmc.ncbi.nlm.nih.gov/articles/PMC3578041/
- Gottfredson, D. C., Najaka, S. S., & Kearley, B. (2007). Effectiveness of drug treatment courts: Evidence from a randomized trial. Criminology & Public Policy, 2(2), 171-196. https://ccjs.umd.edu/sites/ccjs.umd.edu/files/pubs/effectiveness%20of%20drug%20pt%202.pdf
- Marlowe, D. B. (2012). Behavior modification 101 for drug courts: Making the most of incentives and sanctions. National Drug Court Institute. https://ntcrc.org
- Marlowe, D. B. & Meyer, W. G. (2011). The Drug Court Judicial Benchbook. Alexandria, VA: National Drug Court Institute.
- National Institute on Drug Abuse. (2020). Treatment and Recovery. Drugs, Brains, and Behavior: The Science of Addiction. https://nida.nih.gov/publications/drugs-brains-behavior-science-addiction/treatment-recovery
- National Institute of Justice. (2011). Drug Treatment Courts. Office of Justice Programs. https://www.ojp.gov/pdffiles1/nij/238527.pdf
- Substance Abuse and Mental Health Services Administration. (2005). Substance Abuse Treatment for Adults in the Criminal Justice System. Treatment Improvement Protocol (TIP) Series, No. 44. HHS Publication No. (SMA) 13-4056. https://www.ncbi.nlm.nih.gov/books/NBK64137/

